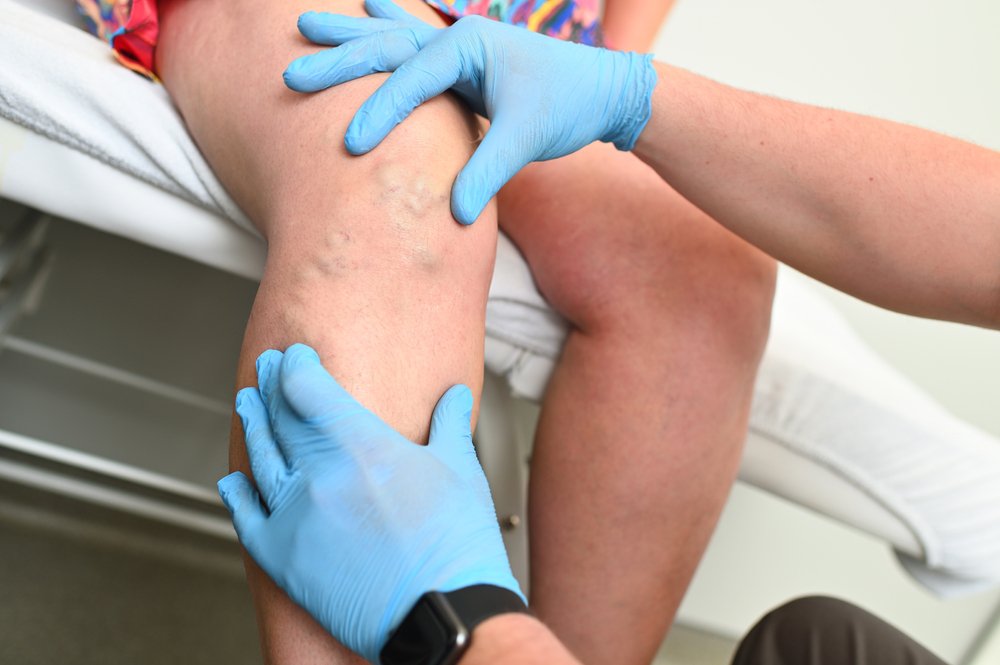
Veins may not be top of mind when it comes to health, but they play a crucial role in your circulatory system. Any issues with your veins can have serious consequences. In this blog post, we will explore common vascular diseases, their symptoms, and available treatment options. But first, let's understand the importance of veins and their impact on overall health.
At ourCenter for Vascular Diseases, our experts treat varicose veins using a technology called radiofrequency ablation, or RFA. RFA is a minimally-invasive procedure that uses heat to close off the affected vein. This method of treating varicose veins is safe, effective, and has a short recovery time.
Varicose Veins
Varicose veins are a common condition in the United States. They occur when the valves in your veins become damaged or weakened, causing blood to pool in your legs and resulting in enlarged and twisted veins. Certain factors increase the risk of developing varicose veins, such as being overweight, having a family history of the condition, or standing for long periods of time. Pregnant women are also more susceptible to varicose veins.
Fortunately, there are ways to prevent and treat varicose veins. Simple lifestyle changes like maintaining a healthy weight and regular exercise can improve circulation and help prevent their development. Avoiding prolonged sitting or standing and wearing loose-fitting clothing can also alleviate pressure on the veins. In some cases, laser treatment or other varicose vein treatment may be recommended to address the symptoms.
While varicose veins are generally not serious, they can cause discomfort, pain, swelling, cramping, and fatigue. In rare cases, they can lead to more severe health issues like blood clots or ulcers. If you experience varicose veins, your doctor may suggest wearing compression stockings or prescribe medication to alleviate symptoms. In severe cases, surgical intervention may be necessary.
Spider Veins
Spider veins, also known as telangiectasia, are a common condition characterized by the appearance of small, dilated blood vessels near the surface of the skin. These veins can cause discomfort and self-consciousness for those affected, leading many to seek spider veins treatment options.
When it comes to spider vein removal, one effective treatment is sclerotherapy. This procedure involves the injection of a specialized solution into the affected veins. The solution irritates the vein walls, causing them to collapse and fade over time. Sclerotherapy is considered a safe and minimally invasive spider vein treatment, with minimal side effects and no need for surgery or anesthesia.
Spider veins occur for various reasons, including genetic predisposition, hormonal changes, prolonged standing or sitting, and certain medical conditions. While they can be more common in women and individuals over the age of 50, spider veins can affect anyone and you should treat spider veins right away.
While smaller varicose veins and spider veins pose mostly cosmetic concerns, larger varicose veins can be indicative of chronic venous insufficiency, a condition where the veins struggle to circulate blood from the legs back to the heart. This insufficient circulation can lead to symptoms such as severe swelling, aching, heaviness in the legs, skin changes, and even open sores called venous ulcers.
If you're looking to treat spider veins, our experts can provide effective spider vein treatment.
Deep Vein Thrombosis
Deep vein thrombosis (DVT) is a condition where a blood clot forms in one of the deep veins, commonly in the leg veins. This occurs when the blood flow in the veins becomes sluggish or interrupted. Various factors contribute to DVT, including prolonged periods of inactivity, excess weight, smoking, and pregnancy.
DVT can result in leg pain, swelling, and cramping. In severe cases, it can lead to serious complications like pulmonary embolism (PE), where a blood clot breaks off and travels to the lungs, causing symptoms such as shortness of breath, chest pain, and coughing up blood. Prompt attention to DVT symptoms is crucial due to the potentially life-threatening nature of PE. Familiarizing yourself with DVT symptoms allows for early treatment if you suspect you have the condition.
If DVT is suspected, it is important to seek immediate medical attention. A doctor will likely perform a physical examination and order tests like an ultrasound to confirm the diagnosis.
Treatment options for DVT vary depending on the severity of the condition. These include the use of blood thinners to dissolve the clot and, in certain cases with large clots or high complication risks, surgery may be necessary. Laser vein treatments, which utilize laser energy to target and treat the affected veins, can also be an option to minimize scar tissue formation. In situations where blood thinners are contraindicated, laser treatments or the placement of an IVC Filter, a metal trap that prevents blood clots from reaching the lungs, may be considered.
Peripheral Arterial Disease
Peripheral arterial disease (PAD) is a condition where the arteries in the legs become narrowed or blocked due to the buildup of plaque, consisting of fat, cholesterol, and other substances in the blood. This plaque can harden over time, leading to the narrowing of arteries and restricting blood flow. PAD is a serious condition that can result in complications like heart attack, stroke, and lower extremity amputations.
Common symptoms of PAD include leg pain or cramping (known as claudication) during physical activity, numbness or weakness in the legs, and non-healing sores or ulcers on the feet or legs. If you suspect PAD, it is crucial to seek medical attention promptly. A doctor will likely conduct a physical examination and order tests such as an MRI or angiogram to confirm the diagnosis.
Treatment for PAD typically involves lifestyle modifications like smoking cessation, regular exercise, and medication to improve blood flow. In some cases, surgical procedures like angioplasty, atherectomy, bypass, or endarterectomy may be necessary. Burst blood vessels and weakened vein valves are complications associated with vascular diseases, emphasizing the importance of maintaining a healthy lifestyle and seeking early intervention.
To prevent vascular diseases, it is essential to follow a healthy diet, exercise regularly, and refrain from smoking. If you have risk factors like high blood pressure or diabetes, working closely with your primary care physician to manage these conditions is crucial in reducing your overall risk.
If you are concerned about these conditions or experiencing any related symptoms, don't hesitate to schedule an appointment with the vascular specialist at Prima CARE. Our dedicated team will provide the necessary care and treatment to ensure your well-being and prevent potential complications.
Don't Let Vein Diseases Vein Your Life - Schedule Your Appointment at Prima CARE Today!
AtPrima CARE, we're proud to offer many services and specialties to our patients. To learn more about our vascular specialists, visit ourCenter for Vascular Diseases website orschedule an appointment today!

